This content is for informational and educational purposes only. Always consult a qualified healthcare provider.
Last Updated on April 1, 2026 by Grace Oluchi
Obesity is more than weight gain. It’s a medical condition where excess body fat begins to affect your health. Doctors often use BMI (Body Mass Index) to check if your weight is healthy for your height, but waist size and lifestyle patterns matter too.
Obesity raises the risk of several health problems, including:
- diabetes
- heart disease
- certain cancers
This is why understanding it early helps you protect your long-term health.
📋 Table of Contents
What Causes Obesity?
Many factors can contribute, and sometimes more than one plays a role.
Genetics
Some people naturally gain weight easily because of how their body stores fat.
Diet
Eating too much processed food, sugar, and unhealthy fats can raise your risk.
Little or No Physical Activity
Not moving enough slows down how your body burns energy. Over time, this allows fat — particularly visceral fat around the organs — to accumulate even if total calorie intake seems moderate.
Calories
If you take in more calories than your body uses, the extra gets stored as fat. This is not always about willpower. Stress, sleep deprivation, and hormonal factors all affect appetite and how efficiently the body burns calories.
Environment
Where you live affects what you eat and how active you are.
For example:
- areas with few parks limit outdoor activity
- places with easy access to cheap snacks push people toward unhealthy choices
The Part Most People Miss: Where Fat Sits Matters More Than How Much You Weigh
Here is something that is not regularly talked about.
Not all body fat carries the same risk. Fat stored just under the skin, the kind you can pinch, is relatively inert. Fat stored deeper inside the abdomen, wrapped around the liver, intestines, and other organs, is a different matter entirely. This is called visceral fat, and it is metabolically active.
Visceral fat releases inflammatory chemicals into the bloodstream, interferes with how the body processes insulin, and directly worsens blood pressure and cholesterol, all at the same time. This is why someone can have a completely normal BMI and still be at a high risk of heart disease. It is also why a person who loses only a moderate amount of weight but specifically reduces waist size can see dramatic improvements in their blood test results.
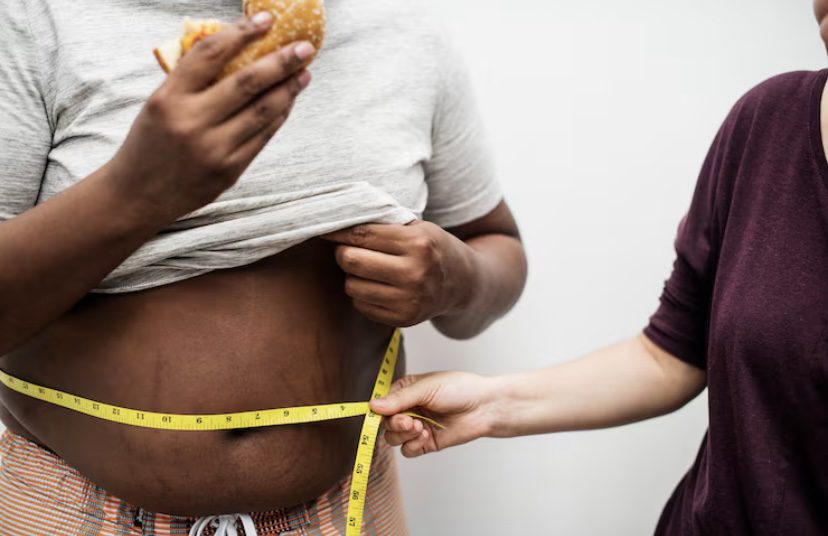
Waist circumference is a more reliable warning signal than weight alone. The NHS uses these as general risk thresholds: above 94cm (37 inches) for men, or above 80cm (31.5 inches) for women, indicates increased metabolic risk. Above 102cm in men or 88cm in women puts you in a high-risk category.
If your waist measurement sits above these thresholds, regardless of what the scales say, it is worth having a conversation with your GP.
Metabolic Syndrome
Metabolic syndrome is a combination of health problems that raise your chances of heart disease, stroke, and diabetes.
You only need three of these to be diagnosed:
- high blood sugar
- excess fat around the waist
- high blood pressure
- low HDL (good cholesterol) or high LDL (bad cholesterol)
Lifestyle habits such as inactivity, poor sleep, and unhealthy eating can make these issues worse. And visceral fat, as we mentioned earlier above, is the common cause driving most of them.
How Obesity and Metabolic Syndrome Connect
Obesity is one of the main risk factors for metabolic syndrome.
Fat stored around the stomach area can:
- affect how your body uses insulin
- raise inflammation
- worsen blood pressure and cholesterol
This combination makes metabolic syndrome more likely to develop.
Managing Obesity and Metabolic Syndrome in a Healthy Way
You can take steps each day to reduce your risk.
Eat better
Choose meals richer in:
- proteins
- veggies
- fruits
- whole grains
- healthy fats like avocado and olive oil
Limit sugary drinks, junk food, pastries, and fried foods.
Move every day
Even 15 minutes daily can help:
- walking
- home workouts
- dancing
- light jogging
Aim for longer sessions as you progress.
Lose some weight
Dropping even 5–10 percent of your current weight can improve:
- blood pressure
- blood sugar
- cholesterol
- energy levels
Manage stress
Try:
- meditation
- journaling
- quiet evening walks
- yoga
- calming hobbies
Follow your doctor’s plan
If you were given medication, take it as instructed.
In some severe cases, bariatric surgery may be recommended.
Prioritize regular checkups
Metabolic syndrome has no obvious symptoms in its early stages. Regular screenings — including blood pressure checks, blood tests for cholesterol and blood sugar, and waist measurements — are how problems get caught before they become serious. Adults aged 40 to 74 in England are eligible for a free NHS Health Check, which covers all of these.
The bottom line
Obesity and metabolic syndrome don’t happen overnight, and they do not have to end in heart disease or diabetes. But they do need to be taken seriously, not just in terms of what the scales say, but in terms of where fat is stored, how the body is functioning, and what the blood test results are showing.
The visceral fat around your middle is not just a cosmetic concern. It is a metabolically active tissue that is quietly affecting your blood sugar, blood pressure, cholesterol, and inflammation levels right now. The waist measurement your GP takes is not a formality, it is one of the most meaningful numbers in the room.
However, with the right habits, the right support, and regular check-ups, you can reduce your risk, improve your metabolic health, and feel meaningfully better over time. Start with the smallest change you can sustain. Build from there.