This content is for informational and educational purposes only. Always consult a qualified healthcare provider.
Last Updated on February 2, 2024 by Grace Oluchi
Purpura is a condition that arises when tiny blood vessels rupture. This issue is more prevalent in individuals whose blood contains low platelet levels, which can be attributed to a base medical condition.
Purpura is a condition that can be caused by a variety of factors, including injury, infections, and medication side effects. However, in some cases, purpura can be a symptom of an underlying autoimmune disorder. Autoimmune disorders are a group of medical conditions that occur when the immune system attacks healthy cells and tissues in the body, leading to inflammation and tissue damage. In this topic, we will explore the common types of purpuras. We will discuss what it looks like, causes, complications and risk factors of it, as well as the treatment options available. We will also address the importance of early diagnosis and management of autoimmune disorders to prevent complications and improve outcomes.
📋 Table of Contents
What is Purpura?
Purpura is a medical condition that results in the appearance of purple or red spots on the skin. The leaking of blood from small blood vessels, leading to the storage of blood beneath the skin causes the spots. The spots can vary in size and shape and can occur anywhere on the body. In some cases, they may also appear on the mucous membranes, such as the mouth or eyes.


There are several types of it, each with different causes and symptoms. One of the most common types is idiopathic thrombocytopenic purpura (ITP), caused by a low platelet count. Platelets are cells in the blood that help to clot the blood and prevent bleeding. When the platelet count is low, bleeding can occur under the skin, leading to the formation of it. Other types include drug-induced purpura, caused by an adverse reaction to medications, and infectious purpura, caused by an infection in the body.
The diagnosis of purpura typically involves a physical examination, a review of the patient’s medical history, and several blood tests. Treatment options depend on the underlying cause of the condition. In cases of ITP, for example, treatment may involve medications to increase the platelet count, while drug-induced purpura may be treated by discontinuing the medication causing the reaction. In all cases, it is important to seek medical attention promptly to ensure an accurate diagnosis and appropriate treatment.
What Does it Look Like?
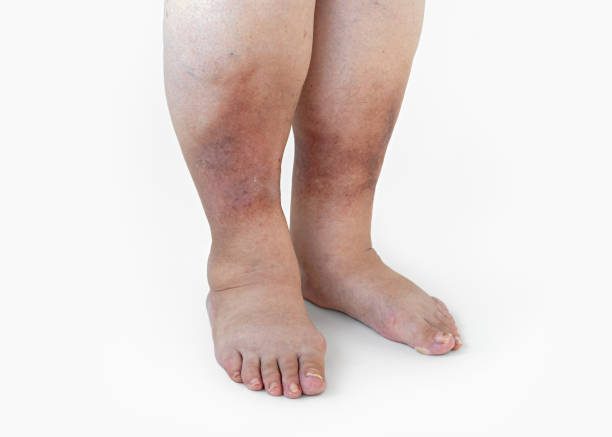

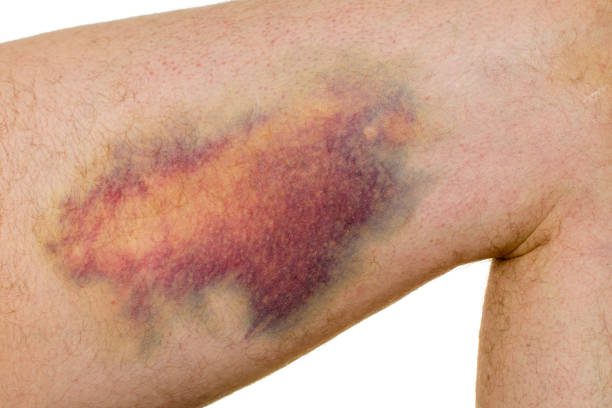
It is a condition in which there is bleeding beneath the skin, resulting in the appearance of purple or red spots. These spots can vary in size and shape, ranging from small dots to larger patches. They may appear anywhere on the body, including the arms, legs, trunk, and face. In some cases, they may also appear on the mucous membranes, such as the mouth or eyes.
The spots caused by purpura are typically painless and do not itch. They may be flat or raised and can sometimes have a blotchy or irregular shape. The color of the spots may change over time, starting out as bright red and gradually fading to a darker purple or brownish color. The spots may also come with other symptoms, such as fever, fatigue, and joint pain.
In cases of severe purpura, the bleeding beneath the skin can be extensive, leading to the formation of large areas of bruising or hematomas. These areas may be tender to the touch and may cause aches or pain. In some cases, the bleeding may also occur in other parts of the body, such as the digestive tract or the brain, leading to more serious complications.
The appearance of purpura can vary widely depending on the underlying cause of the condition and the severity of the bleeding. If you notice any unusual spots or discoloration on your skin, it is important to seek medical attention promptly to ensure an accurate diagnosis and appropriate treatment.
What are the Types?
The two main types of purpuras are non-thrombocytopenic and thrombocytopenic.
- Non-thrombocytopenic purpura occurs due to the increased fragility of the small blood vessels in the skin. Caused by various factors, such as hereditary disorders, blood vessel inflammation, and certain medications. The most common form of non-thrombocytopenic purpura is senile purpura, which occurs in older people due to the thinning of the skin and reduced elasticity of the blood vessels. In non-thrombocytopenic purpura, the bleeding under the skin is not due to a low platelet count but rather due to the fragility of the blood vessels. Treatment for non-thrombocytopenic purpura depends on the base cause, but usually aims to address the factors that add to blood vessel fragility.
- Thrombocytopenic purpura caused by a low platelet count in the blood. Platelets are blood cells that help to form clots and prevent bleeding. When the platelet count is low, bleeding can occur under the skin, leading to the formation of it. There are several types of thrombocytopenic purpura, including idiopathic thrombocytopenic purpura (ITP), caused by a problem with the immune system that destroys platelets, and thrombotic thrombocytopenic purpura (TTP), caused by the formation of small blood clots in the blood vessels. Treatment for thrombocytopenic purpura depends on the base cause and may involve medications to increase the platelet count or other targeted therapies.
What is the Difference Between Petechiae and Purpura?


Petechiae and purpura are both conditions that result in the appearance of purple or red spots on the skin. However, there are some key differences between the two.
- Petechiae are very small, pinpoint-sized spots caused by bleeding from the capillaries. They typically appear in clusters and can be a sign of a serious base condition, such as sepsis or meningitis. Petechiae are not usually painful and may disappear on their own, but tests should always be by a doctor to rule out any serious base conditions.
- Purpura are larger spots caused by bleeding from larger blood vessels. They can range in size from small dots to larger patches and caused by a base medical condition, such as a blood disorder or medication side effect. It may come with other symptoms, such as fever, fatigue, or joint pain, depending on the base cause. Treatment for it depends on the specific cause and may involve medication, lifestyle changes, or other interventions to address the base condition.
Who Can Get it?
Purpura can affect people of all ages, genders, and ethnicities.


However, the incidence and prevalence of it may vary depending on the base cause. For example, non-thrombocytopenic is more common in older adults due to the thinning of the skin and reduced elasticity of the blood vessels. Thrombocytopenic may be more common in children and young adults and caused by an autoimmune disorder or viral infection. Certain medications, such as blood thinners or chemotherapy drugs, can also increase the risk of getting purpura. Overall, anyone can develop it. It is important to seek medical attention if you notice any unusual spots or discoloration on your skin.
What Causes Purpura?
There are two main types of purpura: non-thrombocytopenic and thrombocytopenic. Here are the potential causes of each type:
Non-thrombocytopenic Purpura:
- Aging: Senile purpura is the most common type of non-thrombocytopenic purpura, mainly seen in elderly people due to the thinning of the skin and reduction in elasticity of the blood vessels.
- Blood vessel inflammation: Inflammation of the blood vessels, also known as vasculitis, can cause non-thrombocytopenic purpura. Caused by autoimmune disorders, infections, or medications.
- Hereditary disorders: Some hereditary disorders, such as Ehlers-Danlos syndrome or Marfan syndrome, can cause non-thrombocytopenic purpura due to the added fragility of the blood vessels.
- Sun damage: Chronic exposure to the sun can cause damage to the skin and blood vessels, leading to non-thrombocytopenic purpura.
Thrombocytopenic Purpura:
- Immune system disorders: Idiopathic thrombocytopenic purpura (ITP) is a type of thrombocytopenic purpura caused by an overactive immune system that destroys platelets. Causes can be by autoimmune disorders or viral infections.
- Medications: Certain medications, such as blood thinners or chemotherapy drugs, can reduce the number of platelets in the blood and cause thrombocytopenic purpura.
- Blood disorders: Some blood disorders, such as leukemia or aplastic anemia, can cause a low platelet count and lead to thrombocytopenic purpura.
- Pregnancy: Thrombocytopenic purpura may occur during pregnancy due to changes in the mother’s immune system.
Purpura can be caused by a variety of underlying conditions, ranging from hereditary disorders to autoimmune disorders to medication side effects. If you notice any unusual spots or discoloration on your skin, it is important to seek medical attention promptly to ensure an accurate diagnosis and appropriate treatment.
What are the Risk Factors?
While anyone can develop it, there are several risk factors that may increase the likelihood of getting this condition. Here are some of the most common risk factors:


- Age: As we age, our skin becomes thinner and more fragile, which can increase the risk of getting non-thrombocytopenic purpura.
- Medications: Certain medications, such as blood thinners or chemotherapy drugs, can reduce the number of platelets in the blood and increase the risk of getting thrombocytopenic purpura.
- Medical conditions: Certain medical conditions, such as leukemia, lupus, or other autoimmune disorders, can increase the risk of developing thrombocytopenic purpura.
- Infections: Certain viral infections, such as HIV or hepatitis C, can increase the risk of developing thrombocytopenic purpura.
- Genetics: Some hereditary disorders, such as Ehlers-Danlos syndrome or Marfan syndrome, can increase the risk of developing non-thrombocytopenic purpura.
- Sun damage: Chronic exposure to the sun can cause damage to the skin and blood vessels, leading to non-thrombocytopenic purpura.
- Trauma: Injury or trauma to the skin can cause bleeding under the skin and increase the risk of developing it.
The risk factors for purpura can vary depending on the underlying cause. If you have any of these risk factors or notice any unusual spots or discoloration on your skin, it is important to seek medical attention promptly to ensure an accurate diagnosis and appropriate treatment.
Complications of Purpura.
While generally not a serious condition, it can sometimes lead to complications. Here are some of the most common complications:


- Infection: When the skin is broken due to bleeding, it can increase the risk of infection. This is especially true for people with weakened immune systems.
- Anemia: In severe cases, excessive bleeding can lead to anemia, which is a condition characterized by a low number of red blood cells. Anemia can cause fatigue, weakness, and shortness of breath.
- Organ damage: In rare cases, purpura can cause bleeding in vital organs such as the brain, lungs, or kidneys, leading to organ damage or failure.
- Disability: If caused by an underlying condition such as vasculitis or autoimmune disorders, it can cause long-term disability if left untreated.
- Blood clots: Thrombocytopenic purpura can increase the risk of blood clots, which can lead to serious complications such as stroke or heart attack.
The complications of purpura can vary depending on the underlying cause and the severity of the condition. If you have purpura or notice any unusual spots or discoloration on your skin, it is important to seek medical attention promptly to ensure an accurate diagnosis and appropriate treatment to prevent complications.
Purpura Diagnosis.


To diagnose purpura, a doctor will typically begin by conducting a physical examination to assess the size, location, and appearance of the spots. They may also ask questions about the patient’s medical history and any other symptoms they are experiencing.
In some cases, the doctor may order blood tests to check for abnormalities in clotting factors or platelet levels. This can help identify the cause of the problem with the blood vessels or with the blood itself.
If the underlying cause of it is not immediately clear, the doctor may order additional tests such as a skin biopsy, bone marrow biopsy, or imaging tests to look for any abnormalities in the blood vessels or organs.
The diagnosis of purpura can be complex and may require multiple tests and examinations to identify the underlying cause. As such, it is important to work closely with a qualified doctor to ensure an accurate diagnosis and appropriate treatment plan.
Treatment for Purpura.
The treatment of purpura depends on the underlying cause of the condition. In some cases, it may resolve on its own without treatment. However, in other cases, treatment may be necessary to address the underlying cause and prevent complications.


If caused by a bacterial infection, the treatment may involve antibiotics. In cases caused by an autoimmune disorder, such as lupus or rheumatoid arthritis, the treatment may involve medications to suppress the immune system and reduce inflammation.
If caused by a clotting disorder, medications such as anticoagulants may help prevent blood clots from forming.
In cases where it is related to an underlying medical condition, such as liver disease or kidney failure, the treatment may involve addressing the underlying condition to help improve the symptoms of purpura.
In addition to medical treatments, there are also several lifestyle changes that may help manage the symptoms of purpura, such as avoiding activities that increase the risk of injury or bleeding, wearing protective clothing to prevent injuries, and maintaining a healthy diet and exercise routine.
The treatment of purpura depends on the underlying cause and severity of the condition. It is important to work closely with a qualified healthcare provider to develop an individualized treatment plan that addresses the specific needs of the patient.
When Should a Doctor Treat Purpura?


A doctor should treat purpura if it comes with other symptoms or if it persists or worsens over time. Some signs that medical attention may be necessary include:
- The appearance of large or painful purplish-red spots on the skin
- Unexplained bruising or bleeding
- Development of other symptoms, such as fever, fatigue, or joint pain
- A history of bleeding disorders or other medical conditions that can increase the risk of purpura
- The appearance of purpura after taking medication or following an injury
If any of these symptoms are present, it is important to seek medical attention promptly. A qualified healthcare provider can evaluate the symptoms, perform any necessary tests or examinations, and develop an appropriate treatment plan to address the underlying cause of it.
What is the Outlook for Purpura?
The outlook for it depends on the base cause of the condition. In many cases, it is a temporary condition that resolves on its own once the treatment for the base cause is in action. However, in some cases, purpura may be a sign of a more serious underlying medical condition, such as a blood disorder or autoimmune disease.
If caused by a more serious underlying condition, the outlook may depend on the severity of the condition and the effectiveness of treatment. With prompt and appropriate treatment, management for many underlying conditions can be effective, allowing patients to live healthy and active lives.
The outlook for purpura is generally good, particularly when the underlying cause is identified and treated promptly. However, it is important to work closely with a qualified healthcare provider to manage the condition and prevent complications.
Living With Purpura.
Living with it can be challenging, particularly if the condition is severe or persistent. The condition can affect a person’s physical and emotional well-being and may require ongoing medical management and lifestyle adjustments. Here are some tips:
- Follow a healthy lifestyle: Eating a balanced diet and getting regular exercise can reduce the risk of complications.
- Take medications as prescribed: it is important to take medications with prescription of a qualified doctor.
- Avoid activities that increase the risk of injury or bleeding: Activities that increase the risk of injury, such as contact sports or heavy lifting, avoid them to reduce the risk of bleeding and bruising.
- Wear protective clothing: Wearing protective clothing, such as long sleeves and pants, can help prevent injuries that can lead to it.
- Manage stress: Stress can exacerbate the symptoms, so it is important to practice relaxation techniques, such as deep breathing or meditation, to help manage stress.
- Work closely with a doctor: Regular check-ups with a qualified doctor can help monitor the condition and identify any changes that may require medical attention.
- Join a support group: Joining a support group can provide emotional support and help connect with others who are living with it.
Living with purpura requires ongoing management and attention to the underlying condition. With proper medical care and lifestyle adjustments, people with purpura can lead healthy and active lives.
The Key Takeaway.
Purpura is a medical condition characterized by the appearance of purple or red spots on the skin, caused by bleeding under the skin. The causes is by a variety of factors, including infections, blood disorders, autoimmune diseases, and medication side effects. The treatment depends on the base cause, and may involve medications, lifestyle changes, or other interventions. If purpura persists over time, seek medical attention promptly to identify the causes and get a good treatment plan.
FAQs.
Are there any natural or herbal remedies that are effective for purpura?
While there are no natural or herbal remedies that can cure it, there are remedies that may help manage symptoms:
- Vitamin C: Vitamin C improves the health of blood vessels and may help reduce the risk of purpura. Foods rich in vitamin C include oranges, kiwi fruit, strawberries, and broccoli.
- Bioflavonoids: Bioflavonoids are plant compounds that strengthen blood vessels and reduce inflammation. Foods rich in bioflavonoids include citrus fruits, berries, and green tea.
- Turmeric: Turmeric has anti-inflammatory properties and may help reduce inflammation associated with purpura. It can be consumed in the form of a supplement or added to food.
- Gingko Biloba: Gingko Biloba is an herbal supplement that can improve blood flow and strengthen blood vessels. It is available in the form of a supplement.
Note that natural remedies should not be in use as a substitute for medical treatment. If you have it, it is important to consult with a doctor for proper diagnosis and treatment.
Does purpura hurt?
Whether or not purpura hurts can depend on the base cause and severity of the condition.
In some cases, it may not cause any pain or discomfort. For example, if the condition is caused by a minor injury, such as a bruise it may not be painful.
If caused by a more serious underlying condition, such as an infection, it may be accompanied by pain or discomfort. If caused by a blood clotting disorder, it may be associated with pain and warmth in the affected area.
Does purpura look like a bruise or a rash?
Purpura can look like bruises or a rashes, depending on the size and distribution of the spots on the skin.
Like bruises, it is caused by bleeding underneath the skin, can be caused by lots of factors. Including injuries, blood disorders, infections, and medications. Bruises are caused by a direct impact to the skin, while purpura can appear spontaneously without any apparent injury.
It can also look like a rash, as it often appears as clusters of small spots on the skin. The spots can be flat or raised and may be accompanied by other symptoms, such as itching or burning.
The appearance can vary depending on the underlying cause and severity of the condition. In cases of mild purpura, the spots are small and appear in one area of the body. In more severe cases, the spots may be larger and more widespread, covering large areas of the body.
If you notice any unexplained skin discoloration, it is important to seek medical attention. Your healthcare provider can help determine the underlying cause of the condition and provide appropriate treatment.
What causes purpura?
The causes of purpura can vary depending on the type of purpura. Here are some common causes of purpura:
- Thrombocytopenic purpura: caused by a low platelet count in the blood, caused by infections, medication side effects, and certain cancers.
- Henoch-Schonlein purpura: caused by inflammation in the blood vessels, which can be triggered by infections, medications, or other factors.
- Senile purpura: caused by thinning and weakening of the skin and blood vessels, which can occur with age.
- Allergic purpura: This type of purpura is caused by an allergic reaction to medications, foods, or other substances.
- Trauma-induced purpura: This type of purpura is caused by physical trauma or injury to the skin and blood vessels.
- Infection-induced purpura: Certain infections, such as meningococcal meningitis or sepsis, can cause purpura.
Note that purpura can also be a symptom of an underlying medical condition, such as leukemia, lupus, or vasculitis. If you experience purpura, it is important to seek medical attention to determine the underlying cause and receive appropriate treatment.